All I want for Christmas is to be able to go to sleep – and then not wake up in the middle of the night…
Part 2 of the 5 part series
In my last Christmassy post, I briefly touched on why sleep matters and then hinted at the ‘Elephant in the room’ of dependency forming sedatives. Yikes.
So, let’s (metaphorically) shoot that elephant!
But, where to begin?

Some heavy-duty research in fact, from Kings College London, regarding misuse and MORTALITY for starters:
https://www.kcl.ac.uk/news/investigating-antihistamine-related-misuse-and-mortality-in-england
“New research has found that the proportion of drug-related deaths where first-generation antihistamines were detected ‘significantly increased’ between 1999 and 2019.”
Dated: 23 March 2021 (Accessed 18th Dec 2023)

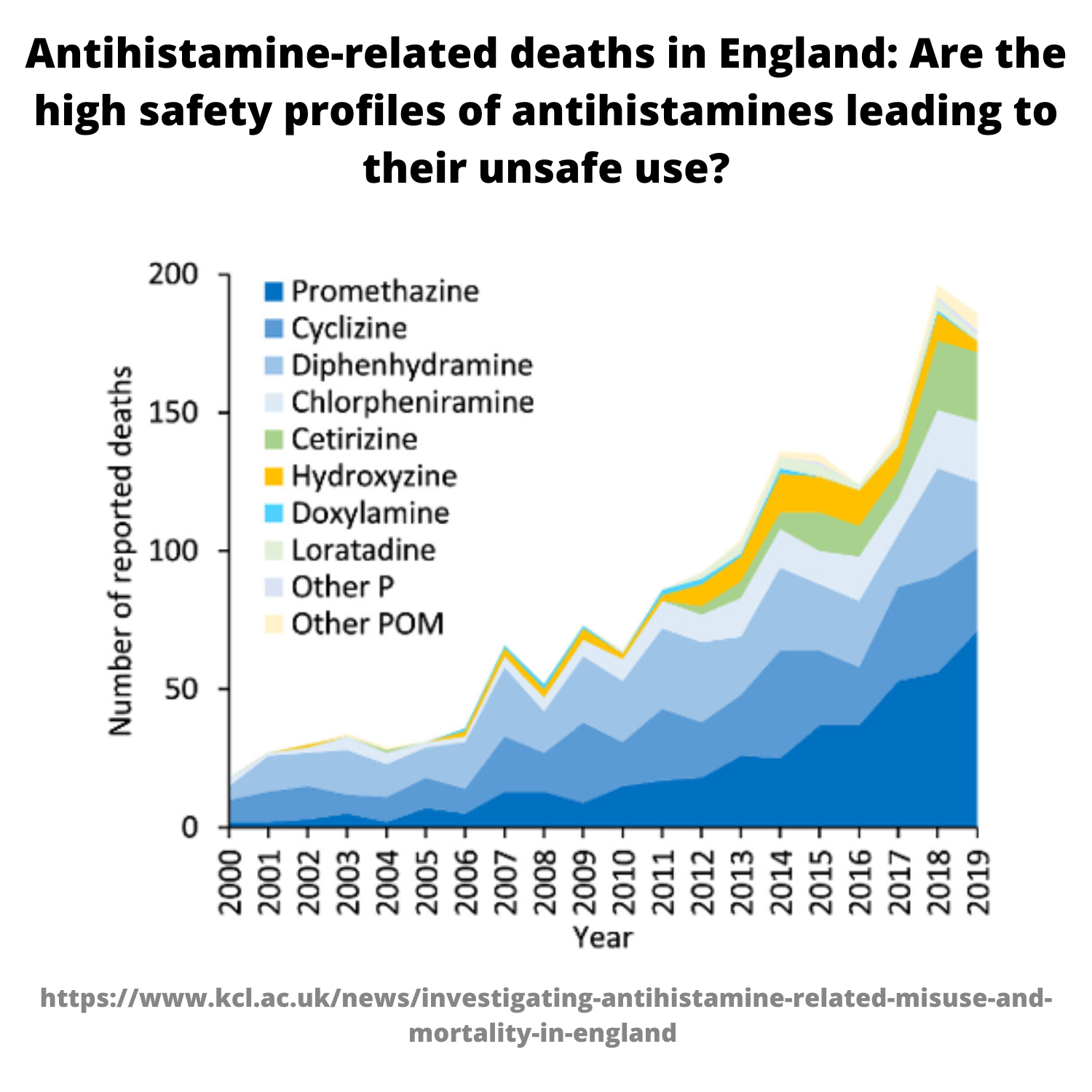
“It is clear that an urgent review of how sedating antihistamines are supplied is needed. Careful consideration will be required to ensure accessibility for those who legitimately use them, whilst restricting use in those deliberately seeking their abuse.”

“Do not recommend OTC treatments for insomnia”.
“How should I manage a person with short-term insomnia (less than 3 months duration)?”
And if we choose to consider ourselves part of Europe… we can add the European Sleep Research Society’s very recently updated (Nov 2023) European Insomnia Guideline. I’ve included the relevant paragraph below:
Therefore, the scientific evidence at this point does not support a recommendation for antihistaminergic drugs in the treatment of insomnia either short or long term. Recently published evidence (Oyekan et al., 2021), indicating an association of antihistamines with increased mortality, suggests further caution.
https://onlinelibrary.wiley.com/doi/10.1111/jsr.14035
Which leads me neatly to:

What IS, a feasible for community pharmacy, first-line therapy for insomnia?
Makes me feel like Lord Nelson, who’s cited as saying:
“I see no ships”.
It’s difficult to see the rows of generic and brand name first generation, sedating antihistamines, typically available in community pharmacy.
But evidence-based, first-line therapy for insomnia, isn’t routinely available at the first HCP/patient interaction, in community pharmacy.
Which is frustrating!
The research is there to demonstrate that CBT-I is effective. It would be a fee-paying option to see a sleep practitioner, so that’s not a viable option on cost grounds for some people and basically there are just not enough sleep practitioners to go round anyway.
An answer could be something as simple as guiding the insomniac to install an app on their phone, known in the typical ‘let’s make it complicated to make it sound important’ way as “Digital Therapeutic Cognitive Behavioural Therapy for Insomnia” or Digital CBT-I.
And it’s even (supposedly) available via the NHS in most of the ICB regions of the UK.
Sadly, the good old-fashioned postcode lottery exists, as to whether in reality you can get it for a patient via their GP.

But did you even know about it?
You no doubt noticed the ‘via their GP’ in the paragraph above.
Were you considered a HCP who should be compensated for their clinical time discussing sleep difficulties?
You only deal with sleep issue patients several times a day and sell countless amounts of sedating antihistamines (I would love to see the sales data if anyone knows how to get it?) – if you’re going to ask me for proof of this ‘assertion’, I suggest you use the evidence of your eyes and take a stroll around a community pharmacy.
So, back to you, the pharmacy team:
Suppose you know about digital CBT-I (a sleep improvement app on your smartphone) how would you make it available?
The big-name brands of digital therapeutic CBT-I have yet to ‘wake up’ (sorry) to the community pharmacy market. I don’t want to upset anyone here, but we really do need to see some action on this.

So, what can you do to help the insomniac?
First get some independent, free, and evidence-based training.
The challenge here is the frustratingly patchy access to NHS digital therapeutics, perhaps a dismissive attitude to an app on a phone, or a private fee-paying sleep practitioner.
The options are…..
Sleepful.me
A free ‘digital therapeutic’ sleep app for insomnia that has evidence to justify its availability.
While perhaps it’s not the most attractively packaged for 2023/2024, it is available for Android and Apple phones here: https://sleepful.me/
The Sleep Reset
Next up, we have The Sleep Reset – it’s a hybrid of a digital therapeutic with the ability to message “a trained sleep coach” for accountability and support.
Could be an option. But only if they can afford to pay for it.
The BSPSS are currently exploring it.
This is an affiliate link:
Sleep Practitioner
If the patient can pay here is where you can find help from a credible source: https://babcp.com/CBTRegister/Search#/
Or you could direct the sufferer to their GP and seek a referral for NHS ‘Talking Therapy’.
Sleeping pills
Happily, we’re seeing a decline in Z drug prescriptions and efforts to deprescribe people from ‘Benzos’.
Scroll down for more about the new alternative.
Pills, pills, pills.
There is a new alternative to the traditional ‘sleeping pill’ that has recently gained MHRA approval. It’s QUVIVIQ (Daridorexant) from Idorsia.
It’s considered not to have the same habituation (dependency forming) and tolerance issues.
https://www.nice.org.uk/guidance/ta922/chapter/1-Recommendations
QUVIVIQ has approval for longer-term insomnia and where CBT-I is not available or unsuitable.
Christmas journey with me now to Part 3




